MicroRNAs (miRs) are small non-coding RNAs that regulate gene expression. Their level of expression is strongly altered in cancer cells compared to normal cells. In addition, miRs are released from many cell types into the extracellular space through highly regulated processes and have been found in a wide spectrum of mammalian body fluids. In recent years, changes in miRNA profiles observed in the bloodstream correlated with various pathological conditions including cancer. Since then, circulating miRs have emerged as promising non-invasive diagnostic/prognostic tools in oncology.
Adrenocortical Carcinoma (ACC) is a rare cancer with poor prognosis and 5-year survival rate of less than 40%. Prognostic evaluation is an essential element in the management of these tumors. The commonly used prognostic factors are tumor extension and intensity of the Ki67 cell proliferation marker. However, prognosis remains heterogeneous among patients and difficult to establish at the individual level. The complexity and heterogeneity of the molecular alterations of ACC are involved in its resistance to conventional and targeted cancer therapies. The best treatment for this highly aggressive tumor remains surgical resection. Poor prognosis is linked to local or distant recurrences (metastases).
Following on from their work on the role of miRs in the physiopathology of this cancer
[1-3], the
new study conducted by IRIG researchers
[4] aimed to evaluate miRs as non-invasive biomarkers (a simple blood sample) that could be used in clinical routine for prognostic evaluation in a short period of time after surgery. Based on their previous work, they quantified the circulating levels of four candidate miRs in serum samples collected within 3 months after tumor removal. They showed that miR-483-5p levels were significantly higher in the serum of patients who had relapsed within 3 years after surgery, as compared to those who had no recurrence
[4]. Statistical analyses revealed that a threshold in circulating miR-483-5p copy number could discriminate between these two groups of patients, with a specificity of 100% and a sensitivity of 61.5%. Patients with miR-483-5p values below this threshold have significantly higher recurrence-free survival (RFS) and overall survival (OS). (Figure). More importantly, a multivariate statistical analysis showed that miR-483-5p is an independent prognostic factor for RFS and OS that performs better than tumor size, ENSAT tumor stage and Ki67 proliferation index.
This study shows for the first time that serum miR-483-5p measured within 3 months following surgery is a powerful biomarker for ACC prognosis. Determination of miR-483-5p circulating levels would improve non-invasive monitoring and personalized treatment of ACC patients. It paves the way for the integration of microRNA assays into routine care.
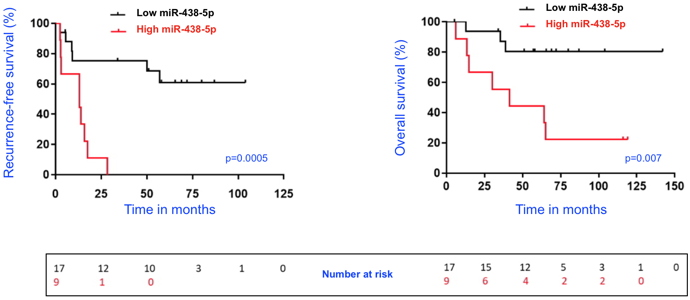 Survival curves of patients with ACC as a function of their post-operative circulating level of miR-483-5p level. Serum was collected within 3 months after surgery.
Survival curves of patients with ACC as a function of their post-operative circulating level of miR-483-5p level. Serum was collected within 3 months after surgery.
A high level of circulating miR-483-5p (High miR-483-5p: number of copies above the threshold defined in the study) is a pejorative predictive factor for recurrence-free survival (high miR-483-5p: median RFS of 1 year; low miR-483-5p: median RFS beyond 8.5 years) and overall survival (miR-483-5p high: median OS of 3.5 years; miR-483-5p low: median OS beyond 12 years).
This study was carried out within the framework of the European Network for the Study of Adrenal Tumors (ENSAT) on a retrospective cohort of 48 patients who were not metastatic at diagnosis and were operated on at the University Hospital of Würzburg (Germany).